Abstract
Introduction: The multifactorial and complex pathophysiology of pulmonary embolism (PE) involves dysregulation of hemostatic system including fibrinolytic imbalance, endothelial compromise and generation of thrombotic mediators, along with cellular defects and hemodynamic derangement. It is estimated that 6000 cases of pulmonary embolism and DVT are reported yearly of which 1000 result in death. PE evolves from a pre-existing venous thrombus, obstructing pulmonary artery leading to pulmonary failure. The progression of clot formation results in increase in right ventricular pressure, systemic hypoperfusion, hypoxemia ischemia and eventually multi organ failure. Fibrinolytic dysregulation and generation of procoagulant mediators result in increased clot burden and lead to adverse outcomes. Profiling of the component of the fibrinolytic system for such mediators as the activators and inhibitors of fibrinolysis, vWF and cellular microparticles may provide additional insights into the pathogenesis of PE. The purpose of this study is to profile plasma samples from PE patients for various mediators of hemostatic dysregulation which contribute to the fibrinolytic dysregulation in PE patients.
Material & Method: Seventy-eight patients of 18 years or older age, were included in this study through enrolment conducted in conjunction with an ongoing IRB approved project by the pulmonary embolism response team (PERT) registry. Diagnosis of PE was confirmed by computed tomography (CT), angiography or ventilation perfusion imaging. Blood samples were drawn with in 24 hours of confirmed diagnosis of acute PE in 3.2% sodium citrate tubes at the time of diagnosis, processed for platelet poor plasma and frozen. Control plasma samples were obtained from 50 healthy individuals. Both the patient and control plasma samples were analyzed for D-Dimer, PAI-1 antigen, tPA, TAFI-a, protein C, alpha-2 antiplasmin, microparticles and vWF using ELISA methods (Hypen Biomedical, Franklin, Ohio). A functional PAI-1 chromogenic substrate method and an ELISA based uPA antigen method was used (Biomedica, Halifax, Nova Scotia, Canada). Circulating levels of each of the individual biomarkers were compared to normal plasma, descriptive statistics including non-parametric Mann-Whitney t-test and spearman correlation coefficient analysis was carried out by using GraphPad Prism software. Percent Increase from the normal mean was calculated for each individual parameter. p value <0.05 was considered statistically significant.
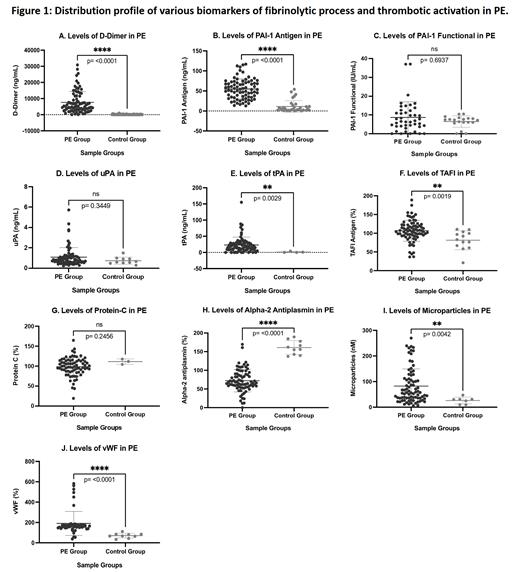
Result: In comparison to normal group, the PE patients exhibited varying levels of increase in the D-Dimer, tPA, uPA, PAI-1 antigen, PAI-1 functional, TAFI antigen, microparticles and vWF, whereas decreased levels were noted for protein C and alpha-2 antiplasmin as shown on Figure 1. D-Dimer showed the most pronounced increase (368.2-fold) followed by tPA (165.9-fold), PAI-1 antigen (3.91-fold), microparticles (2.14-fold), vWF (1.83-fold), uPA (0.5-fold), TAFI antigen (0.40-fold) and PAI-1 functional (0.34-fold). In correlation analysis, D-Dimer negatively correlated with TAFI antigen (r= -0.3106) and alpha-2 antiplasmin (r= -0.3056), functional PAI-1 levels positively correlated with tPA (r= 0.3117) and protein C (r= 0.4059), tPA negatively correlated with TAFI antigen (r= -0.4601), alpha-2 antiplasmin (r= -0.2460) and positively correlated with microparticles (r= 0.2456) , TAFI antigen positively correlated with protein C (r= 0.3612), alpha-2 antiplasmin (r= 0.3899) and negatively correlated with microparticles (r= -0.2470) whereas protein C showed a negative correlation with vWF (r= -0.2838).
Conclusion: The markedly increased D-Dimer levels suggest increase clot burden in PE patients. tPA antigen is also markedly increased, whereas the uPA showed modest increase which may suggest compensatory upregulation, PAI-1 antigen levels were much higher in comparison to PAI-1 functional activity, suggesting consumption of this inhibitor. Decreased alpha-2 antiplasmin and protein C levels also suggest consumption. Increased TAFI antigen contribute to the clot resistant to fibrinolysis. Cellular consumption and endothelial dysfunction results in increased in vWF and microparticles promoting thrombogenesis. Measurement of these biomarkers may be useful in the understanding of the pathogenesis, risk stratification and clinical management of PE patients.
No relevant conflicts of interest to declare.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal